About Knee
- Home
- Patient Info
- Knee
About Knee
Your knees may develop problems like pain, swelling, instability, locking or general difficulty in walking, climbing stairs and running. Common causes for these problems are cartilage and ligament injuries as well as arthritis or wear-tear of the knee.
There are many causes of knee pain – common ones are outlined below. At “The Joint Clinic” we tailor make solutions. Simple problems are treated by medication and exercises.
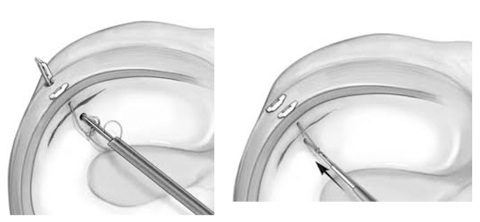

Meniscus Tear
A meniscus tear is a common knee injury, it may be the most common knee injury. The meniscus is a rubbery, C-shaped disc that cushions your knee. It can be thought of as the shock absorber of the knee. Each knee has two menisci – one at the outer edge of the knee and one at the inner edge. The menisci keep your knee steady by balancing your weight across the knee. A torn meniscus can prevent your knee from working right.
Knee Pain from meniscus (shock absorber) tears is usually the result of a twisting injury. When the menisci are weakened due to aging, they may tear even with trivial events such as a false step while walking. Complaints are pain or clicking in the knee. The knee may sometimes lock and it becomes impossible to bend or straighten it.
The diagnosis is made by doing a detailed examination of the knee, followed by X-Rays and MRI Scan of the knee.
Treatment is by arthroscopy (keyhole surgery). In most cases, the torn meniscus is removed. This can be performed under local or spinal anesthesia. More about Knee Arthroscopy.More about arthroscopy in Local anesthesia
In young patients, the meniscus is sometimes amenable to repair. This is also carried out by arthroscopic techniques. More about meniscal repair
Cartilage Tear
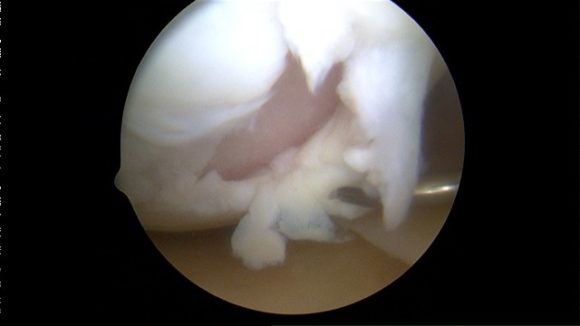

There are areas of cartilage tissue covering the ends of the long bones at the knee joint – these are called articular cartilages. Tough connective tissue (articular cartilage) covers the ends of the tibia and femur and the back of the patella around the knee joint. The articular cartilage reduces friction between the bones of the knee joint and helps smooth movement between them. These areas of cartilage may become damaged causing significant problems for patients. Knee Pain from Cartilage tears can result from injury or overuse. Damage to the cartilage covering the end of the bones at the knee joint is called a chondral injury. If the underlying bone itself is also damaged, this is called an osteochondral injury. Common complaints are pain, swelling, clicking and difficulty walking.
Examination of the knee may reveal a swelling of the joint, a ‘crunching’ of the joint or locking. X-rays are sometimes useful but an MRI scan provides doctors with the best pictures of the articular cartilages of the knee.
Minor tears can be cleaned with arthroscopy. Bigger ones require microfracture – an arthroscopic technique of making small holes in bone following which cartilage regenerates. More about microfracture
Large cartilage defects have to be managed by grafting cartilage from other parts of the knee along with bone plugs. More about osteochondral grafting
Some patients with cartilage tears may be suitable for cartilage transplant. In this technique, a part of cartilage is taken from your knee, then in the lab that cartilage grows into a big piece which is then transplanted back into your knee. More about cartilage transplant
Knee Ligament Injuries
A ligament is a tough strip of connective tissue that joins one bone to another bone around a joint. The knee joint ligaments help to stabilise and support the knee when it is moved into different positions. There are four main ligaments in the knee that can become injured. During injury, a knee ligament may be stretched (sprained), or sometimes torn (ruptured). Ligament rupture can be partial (just some of the fibres that make up the ligament are torn) or complete (the ligament is torn through completely).
Knee ligament injuries can cause pain, swelling, tenderness, bruising and reduced movement of your knee. Your knee joint may feel unstable and you may walk with a limp. Treatment of a knee ligament injury can depend on a number of things including which ligament is injured and how sporty and active you are.
Each ligament has a different job to do:
- The medial collateral ligament (MCL) is one of the ligaments on the inside of the knee joint. It helps to protect and stabilise the knee joint against any forces on the side of the leg. It helps to limit the amount that the knee moves from side to side. Injuries to the MCL can happen in almost any sport. They often happen when your leg is stretched out in front of you and the outer side of your leg receives a blow at the same time – for example, during a football tackle.
- The lateral collateral ligament (LCL) is the other main ligament on the other side of the knee joint. It helps to protect and stabilise the knee joint against any forces on the side of the leg. This ligament also helps to limit the amount the knee moves from side to side. Injuries to the LCL are less common than injuries to the MCL. This is because your other leg usually protects against injury to the inner side of your knee.
- The anterior cruciate ligament (ACL) is one of the ligaments inside the knee joint. It runs diagonally connecting the front (anterior) of the tibia to the back (posterior) of the femur. This ligament helps to stabilise the knee joint by controlling backward and forward movements of the knee. It stops the tibia bone from moving forwards in front of the femur. ACL injuries most often occur during sports. The injury happens if you land on your leg and then quickly pivot or twist your knee in the opposite direction while it is slightly bent. Women are more likely than men to injure their ACL. About half of people with an ACL injury also have injury to their meniscus or another ligament in the same knee.
- The posterior cruciate ligament (PCL) is the other ligament inside the knee joint. It also runs diagonally across the knee, connecting the back (posterior) of the tibia to the front (anterior) of the femur. The ACL and PCL cross each other inside the knee joint and some people call them the cross ligaments (cruciate means cross-shaped). The PCL helps to control the forward and backward movements of the knee. Injuries to this ligament are not as common as ACL injuries. This is because the PCL is wider and stronger than the ACL. Your PCL can be injured if your leg receives a direct blow from the front.
If you feel that you may have a knee ligament injury, you should see a doctor. Your doctor will examine your knee by moving your leg into different positions to test your knee ligaments. From this examination, they may be able to get an idea of the possible injury that you have. Further tests such as an MRI scan is almost always needed. Such tests should be able to show up any tears or rupture of your ligaments. Sometimes, an X-ray of your knee may be suggested, if they suspect a fracture.
Most common ligament to tear is ACL (anterior cruciate ligament). We perform Anatomic ACL reconstructions where the graft restores your ligament exactly from where it came off. This is an arthroscopic or keyhole procedurewhich helps you get back to sports.More about ACL Reconstructions
Similarly PCL, MCL, PLC ligament tears can be repaired or reconstructed to restore your active lifestyle. We also perform multiple ligament reconstructions for badly injured knees with excellent outcomes. More about ligament injuries
Anterior Knee Pain or Patello-Femoral Pain
Patellofemoral pain syndrome is used to describe pain in the front of the knee and around the kneecap. It is sometimes called “runner’s knee” or “jumper’s knee”. The pain and stiffness it causes can make it difficult to climb stairs, kneel down, and perform other everyday activities. Many things may contribute to the development of patellofemoral pain syndrome. Problems with the alignment of the kneecap and overuse from vigorous athletics or training are often significant factors.
The most common symptom of patellofemoral pain syndrome is a dull, aching pain in the front of the knee. This pain usually begins gradually and is frequently activity-related. Other common symptoms include pain during exercise and activities that repeatedly bend the knee, such as climbing stairs, running, jumping, or squatting, pain after sitting for a long period of time with your knees bent, such as one does in a movie theatre.
Symptoms are often relieved with conservative treatment, such as changes in activity levels or a therapeutic exercise program. Initial treatment is with exercises. Sometimes arthroscopic surgery is required to realign the kneecap. This cures the pain completely. More about arthroscopic lateral release
Normal Patella
Maltracking Patella
Maltracking Patella
Recurrent Patellar Dislocations
Patellar dislocation occurs when the patella or kneecap slips out of its groove on the front of the lower end of the femur (thigh bone). A subluxation is a partial dislocation in which the patella slips but immediately goes back into place. In a true patellar dislocation the patella goes back into place as a distinct movement, usually when the knee is straightened. When a patella dislocates the chance of another dislocation is quite high, somewhere between 15% and 45%. The specific risk is greater if there are associated predisposing factors such as the alignment of the leg, the shape of the groove in the femur for the patella, how high the patella sits in relation to the rest of the knee joint, and the alignment of the foot and ankle. When the patella dislocates on more than one occasion the term recurrent patellar dislocation is used. After two dislocations, the risk of further episodes of dislocation is very high, somewhere in the order of 60% to 80%
Typical symptoms can include severe swelling, pain around the knee cap, and/or a feeling like dislocation may happen again. However, pain and swelling may not accompany dislocations if they occur easily and the cartilage is not damaged.
Knee cap dislocations can be either managed by tightening the ligament (MPFL) which keeps the knee cap in its place or by moving the part of shin bone where the knee cap attaches.
Loose Bodies in the knee
Loose bodies in the knee joint are small fragments of cartilage or bone that move freely around the knee in joint fluid, or synovium. They can hinder the joint moment by getting caught in flexion and extension movements. The loose bodies can vary in size from a few millimeters to a few centimeters. The fragments can lead to damage to the articular cartilage, causing osteoarthritis.
The common causes leading to formation of loose bodies are injury to cartilage during trauma or sports, osteoarthritis or Charcot’s disease, fibrinous loose bodies in inflammatory conditions of knee and/or synovial chondromatosis (also called synovial osteochondromatosis) in which the synovium grows abnormally and produces nodules made of cartilage.
Common symptoms are feeling of something moving in knee and/or knee locking as though something is blocking it. Examination and diagnosis is by X-ray, and MRI – when the loose body is just cartilage or in the case of synovial chondromatosis, a MRI is the best non radiation diagnostic tool to asses the whole knee joint. It is a useful preoperative tool to see size, number and location of the loose bodies. Sometimes, a CT scan may be needed for the diagnosis.
There are limited options of non-surgical management of a loose body as it mainly leads to mechanical symptoms which are relieved only after removal. Arthroscopy is the gold standard today.
Loose Bodies
Loose Bodies
Knee Arthritis
It is a common condition that causes pain and swelling in the knee joint. It can start after injury or with advancing age due to “wear and tear”. Certain diseases like rheumatoid or gout can also trigger knee arthritis.
Early stages can be treated with pain killers, exercises, activity modification and joint injections. More advanced cases need surgery.
Sometimes it is possible to preserve half of the knee by doing a Unicompartmental Knee Replacement. But more often the surgery of choice is a Total Knee Replacement. We specialize in cruciate retaining knee replacements, which keep your posterior cruciate ligament intact during surgery. This minimises required bone cuts and preserves your tissues thereby giving a more natural feel in your replaced knee. With enhanced recovery techniques you can walk the next day and can go home after 48-72 hours. More about Knee Replacements about Knee Replacements
Knee Stiffness
Knee stiffness develops after injury, surgery, prolonged immobilisationeg in a plaster or following an infection. Early cases are managed with physiotherapy. Advanced cases need surgery called arthrolysis to free up the joint. This can be performed by arthroscopic techniques.
